|
Some things to consider bringing with you to work during #COVID19
PDF Poster on how to help ICU Staff during #COVID19 You can find all the resources for NON-ICU Staff, here. PDF Below.
Created and developed by my Irish colleague Dr. Bryan Reidy (@bryan_reidy) and used locally at his hospital (Beaumont). These are NOT definitive resources and may NOT be suitable for your purposes. This is an educational resource only. By downloading, you accept the disclaimer on Propofology.com 1. ACLS/ALS in ICU 2. ACLS/ALS whilst PRONED 3. ACLS/ALS on the WARD 4. ACLS/ALS Checklist 5. FAST HUGS (Daily ICU Checklist) 6. Haemodynamics 7. Prone 8. Sedation 9. Standard Orders 10. Support for Staff 11. Ventilation and Weaning PDF Views below gallery. Full Zip File PDF Download
Intended to be an editable resource.
Have included PDF's or Power Point so you can edit them to your needs and print as needed. I hope these help.
Initially this booklet was designed for those about to be put onto the ICU rota (usually anaesthetic trainees). Now this booklet is also written considering the potential heath crises we face with the arrival of COVID-19 to Ireland. All credit to Dr. Peter McCauley (Ireland) for this eBook and for making it available as #FOAMed.
General considerations about #COVID19
Summarised from a variety of sources including: www.cdc.gov www.gov.uk www.who.int www.emcrit.org/ibcc/covid19/ www.esicm.org/resources/coronavirus-public-health-emergency/
Full Screen Versionhere
Here is my full Tweetorial on Coronavirus. Updated as more evidence emerges.
Focuses on the fundamentals and then goes on to specific recommendations by @ICS_Updates and the Dept of Health (UK) on its potential impact to Intensive Care. CLICK HERE
A glance at the literature from 2010-2018
A growing body of evidence and expert reviews suggests that we should be altering our administration regimes of beta-lactam and carbapenams to accommodate an altered volume of distribution (or RRT) status of the critically ill patient in order to more effectively reach the inhibitory concentrations of drug required to kill susceptible pathogens. Don't forget you can catch the full trials at pubmed.gov and enter the PMID within the infographic. HD FULLSCREEN HERE PDF at bottom of page
PDF included at bottom of page for a clearer graphic (incl. 811 references!)
Fullscreen of the graphic below: here.
Dr. Sergey Motov (USA Emergency Medicine) & Dr. David Lyness (UK ICM/Anaesthetics)
UPDATE - NOVEMBER 2018 Taken from Dr Motov's work on a CERTA regime. This is published in conjunction with the CERTA concept explanation here. We can all provide superior analgesia by using medication and techniques other than just opioid medications. This is NOT a definitive list and in all cases, local policies and protocols should be followed. Check your local formularies. This is NOT a prescribing guideline - it is for EDUCATIONAL information ONLY. We do not dispute the role of opioids in many spheres of practice, including emergency medicine, ICU and anaesthetics; rather we wish to highlight the pandemic of high opioid and opiate use. There are many medications available to reduce the amount of opioids used. You may find, when considering your analgesia regimes that opioids are not always the best options for emergency pain issues. We would advocate the use of nerve blocks in the first instance to control acute pain, when feasible.
With respect to alternatives listed for non-radicular back pain, it has been brought to our attention that a new study was presented in 2017 which showed that "diazepam has no benefit when added to naproxen vs placebo" in acute low back pain. See here.
This is a difficult document to see online - so I have included a fullscreen version here and the A3 printable PDF below.
There were 811 references when compiling this document; they can be found below....
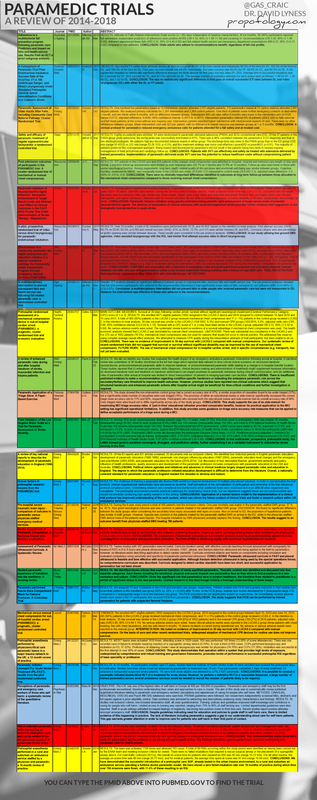
PDF at bottom of page for best quality version. Fullscreen HD here. ALL of the trial abstracts are on PubMed.gov and can be found quickly by typing the PMID found in the reference below into its search field.
PLEASE let me know if you see any errors and I will try to fix them ASAP.
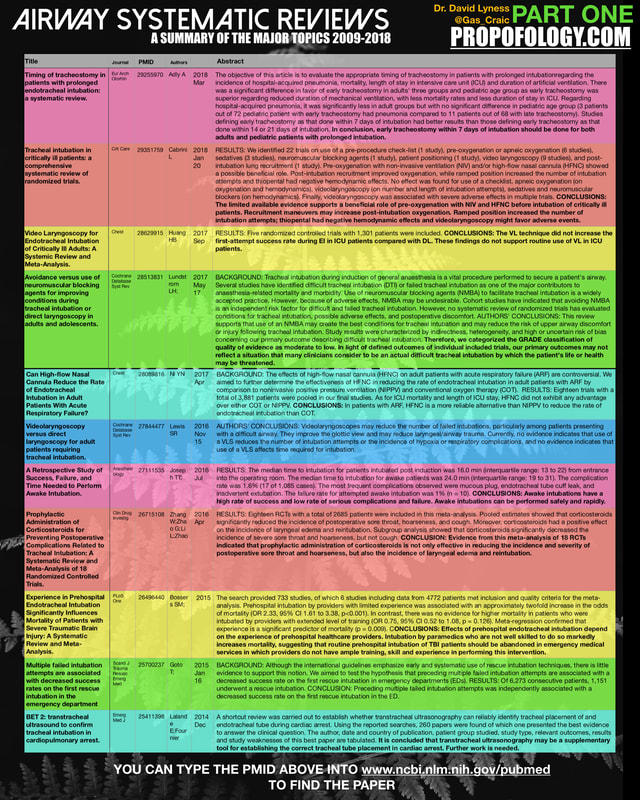
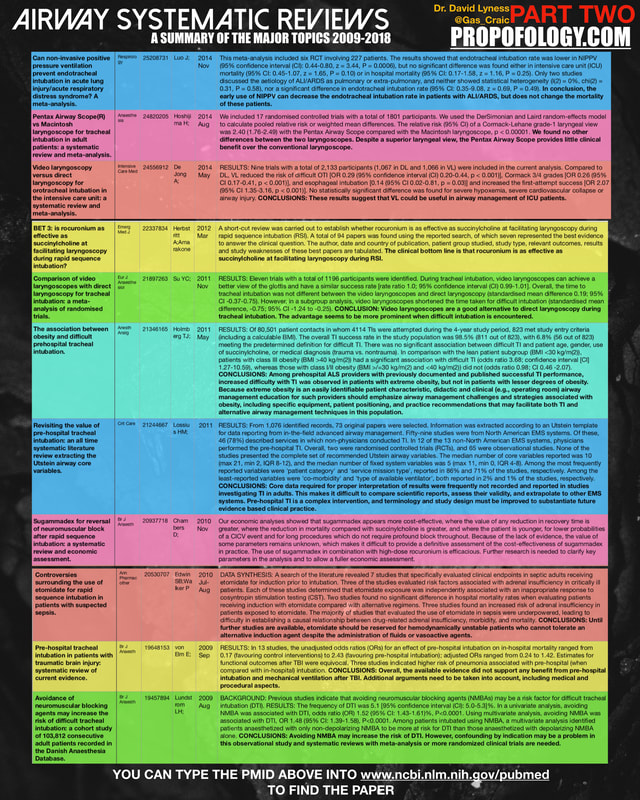
HD Fullscreen of the infographs are at the bottom PDF at bottom of page I preface this infographic with the caveat that it is an exercise in discussion only, not an exhaustive or conclusive analysis of all systematic reviews within this time period. I have done my best to accurately analyse the trawled data - please do get in touch if you have any suggestions on improvements. I have no conflicts of interest and am not involved in any systematic reviews or trials with any organisation.
These studies were found on PubMed and are ONLY the ones with completely #FOAMed access.
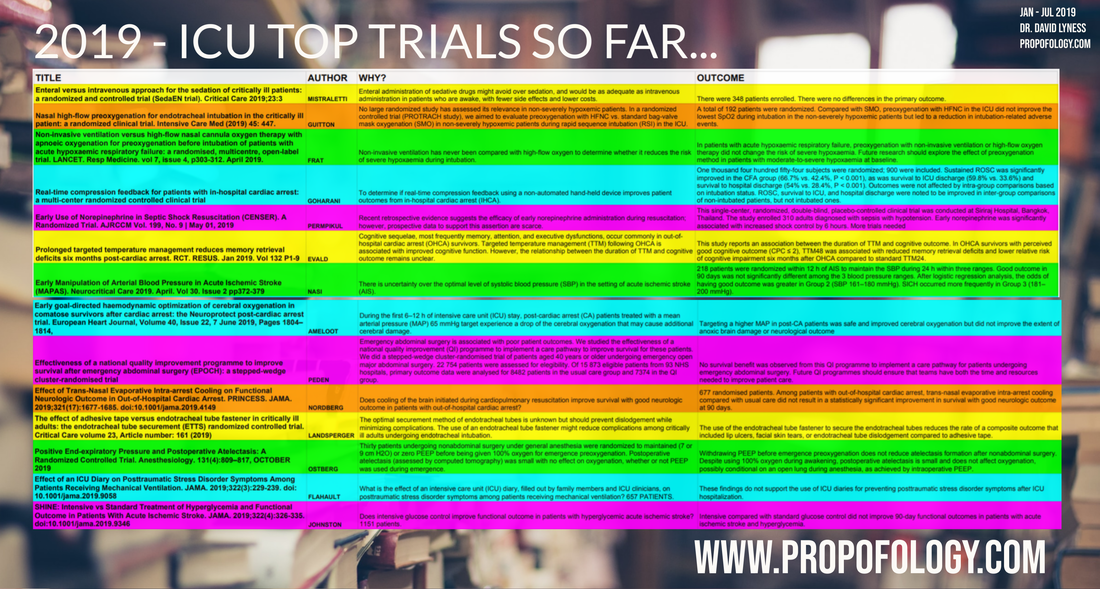
Interactive Version: FULLSCREEN HERE (HD Quality) PDF file below SEE ALL MY TRIAL SUMMARY DOCUMENTS HERE!
Interactive Version.
PNG Picture. PDF at bottom.
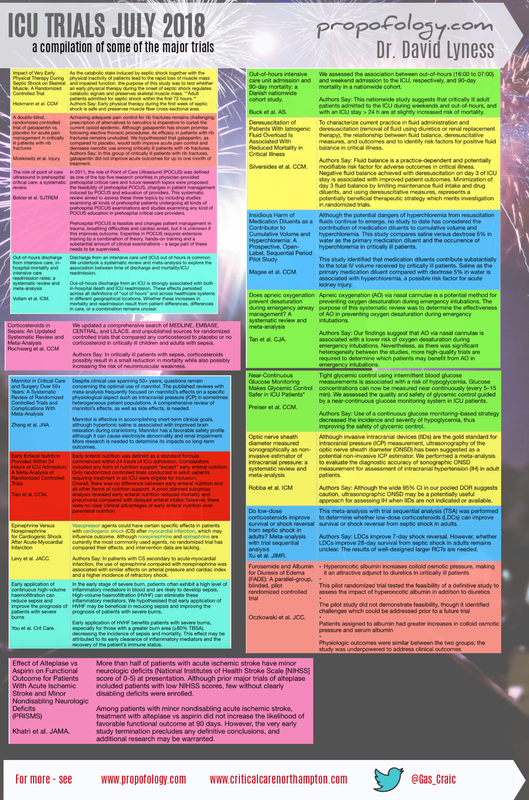
A busy month, but a snapshot of some of the ICU trials of July 2018! (Clearer graphic in the PDF below)
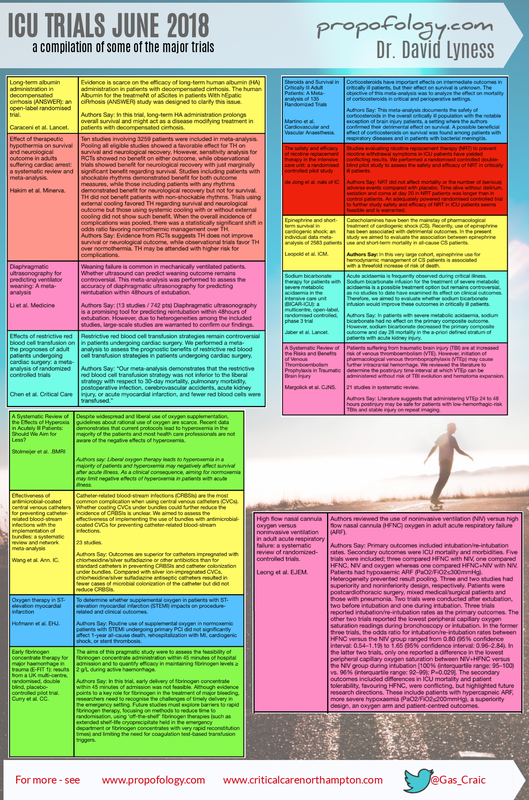
A snapshot of some of the major journal articles/trials in MAY 2018 for ICU
Enjoy!
A snapshot of some of the major journal articles/trials in April 2018 for ICU
Enjoy!
FULLSCREEN
DOWNLOAD BELOW:
A snapshot of some of the major journal articles/trials in March 2018 for ICU
Enjoy! FULLSCREEN PDF DOWNLOAD (free) |
USE OF THIS WEBSITE IS SUBJECT TO AGREEING TO THIS DISCLAIMER
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||

Free to access Propofology Infograms, eBooks and selected YouTube videos by Dr. David Lyness are licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Please attribute all works: 'Based on a work by Dr. David Lyness' at www.propofology.com/resources.
|
Home
About Contact |
ALL SITE USERS SHOULD READ AND AGREE TO THE DISCLAIMER HERE.
Contact via Twitter |










 RSS Feed
RSS Feed